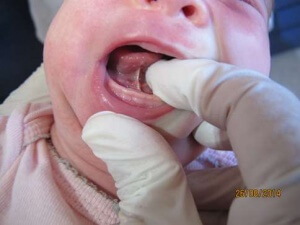
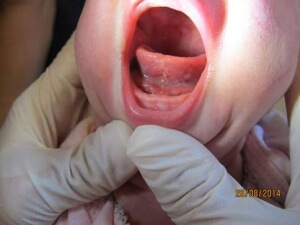
The procedure
- Local anesthetic gel can be applied under the tongue – for infants older than one month or at the parents’ request
- The frenulum is released with sterile scissors that have been autoclaved.
- In case of bleeding, gentle pressure is applied with a sterile gauze.
- The baby is brought back to mother for feeding immediately after the procedure
- If the baby is not breastfeeding, or does not latch on for any reason, application of breastmilk to his mouth is possible. Breast milk facilitates wound closure and faster healing and helps calm the baby.
Possible risks
- Bleeding – can be treated medically. Additionally, breastmilk has a good effect on hemostasis.
- Infection – to prevent this we use sterile tools that are sterilized to the highest degree.
After releasing the tongue
To prevent future infection – ensure that all hands that touch the baby are thoroughly washed and prevent young siblings from coming in contact with the baby’s mouth.
Recommendations following the tongue release – If the baby is fully breastfeeding: Frequent breastfeeding for the first two days to ensure the baby’s quick adjustment to its “new tongue”.
Please keep us updated during the first 24 hours after the tongue release and let us know how breastfeeding is going.
If the baby was having breastfeeding challenges prior to the tongue release, skilled lactation assistance may be required in order to get breastfeeding back on track.
Stretching Exercises – to prevent the reattachment of the frenulum: These are done for a week, three times a day. Each time, the parent passes his finger three times under the width of the baby’s tongue, and lifts the baby’s tongue from underneath, at the place of the release, using the forefinger (3 times).
The healing of the incision – in some cases (posterior tongue tie), following the procedure, a white coating (in the shape of a diamond) will appear under the tongue; this is part of the healing process and is not pus. Do not attempt to remove it and continue doing the exercises.
Pain – most babies do not show signs of pain following the procedure of tongue release. If it seems there is need, pain medication such as paracetamol may be given according to directions on the packaging of the medication. It is important to prevent pain (if it appears), in order to enable the exercise of the tongue while nursing and thus quickly improv the movement of the tongue following the release.
Fever – there should not be any fever rise following the procedure, however if the baby’s fever rises, notify the attending physician.
Bleeding – There should not be bleeding following the procedure. However, if there is heavy bleeding, notify us immediately. We will give you instructions. Light bleeding may appear while doing the post-operative exercises may be noted if the baby spits up, or in the baby’s stools, due to the baby swallowing some blood during the procedure.
Wishing you and your baby a quick recovery,
Dr. Gina Weissman
and the HalavM professional staff
Written by Ariela Levy Breastfeeding Management Course 2014
Translated from Hebrew to English by Judy Ronen
HalavM breastfeeding Clinic